Population health and inequalities in Edinburgh
This topic paper provides a brief overview of population health in Edinburgh with particular emphasis on inequalities. Unless otherwise stated all health data in graphs and tables has been produced by the Public Health Scotland’s Local Intelligence Support Team (LIST) utilising routine data held by Public Health Scotland.
This paper starts with a brief summary of high-level mortality and life expectancy data. The paper adopts a life course approach and references data to illustrate health and inequalities trends and the way that they impact different age groups. A data appendix provides more detail about specific diseases and risk factors.
There are nine sections in this paper considering
- Factors that influence population health and inequalities
- Early years and health inequalities
- Life expectancy in Edinburgh
- Mortality and morbidity
- Healthy life expectancy and quality of life
- Multimorbidity
- Loneliness and isolation
- Age, sex and hereditary factors
- Behavioural risk factors.
The paper does not include detailed analysis of the health impacts of COVID-19 in part because complete data for the impacts on Edinburgh’s population are not yet available. Initial analysis highlights that the pandemic has exacerbated existing health and social inequalities.[1-3] Those in insecure employment, unable to work from home, experiencing digital exclusion, lacking financial and other resources such as their own transport, are worst equipped to follow isolation and distancing guidelines. In turn this means they are both more exposed to and more susceptible to the negative social and health impacts associated with COVID-19.[4]
Age is a risk factor for severe COVID-19 illness along with a number of underlying health conditions. Males, people aged 70 years and older, people working in lower paid jobs[5-7] and people from some ethnic minority groups are more likely to die from COVID-19 than other population groups.[8-12] The most recent data from National Records of Scotland indicate that people from the most deprived communities are 2.4 times more likely to die from COVID-19. [13] There is evidence of longer-term health complications from COVID-19, including Long COVID. [10, 14-16] While children and young people have been far less affected by the direct impacts of the pandemic in terms of severe morbidity and mortality, they have been disproportionately affected by the wider impacts including lockdowns and longer term economic implications. These impacts are exacerbating existing inequalities amongst children and young people.
COVID-19 has also directly impacted the life circumstances of the Edinburgh population in differential fashion. Unemployment, loss of income and challenges associated with caring responsibilities are socially patterned. The burden of social impacts associated with COVID-19 has been disproportionately borne by women, notably in terms of loss of income and jobs and increased childcare and domestic responsibilities. There is some evidence of increased domestic abuse and research shows that women’s mental health has worsened during the pandemic.[17-20] The impacts of institutional racism – poorer housing conditions, lower paid jobs, more unemployment – manifest themselves in terms of greater risk from COVID infection and a harder financial and social impact associated with loss of income and unemployment. Crucially, the higher mortality risk for people from ethnic minority groups is not explained by biological differences but social determinants.[2, 8, 9, 21-23].
- Edinburgh is more affluent than other parts of Lothian and its population generally has better health. But health inequalities in Edinburgh are significant especially when compared with Lothian and Scotland.
- The difference in life expectancy between people living in the most deprived areas and the least deprived areas is 10 years for females, and 14 years for males.
- The life expectancy gap between females and males narrows from 5.8 years in the most deprived area to 2.3 years in the least deprived area.
- Females in Edinburgh experience fewer years of good health than males.
- There is evidence of a widening gap between males and females which appears to be a combination of improvements in male healthy life expectancy and a worsening of female healthy life expectancy. Although females have a higher life expectancy, they spend more than 20% of that life experiencing poorer health.
- There is evidence of declining life expectancy among some population groups since 2013.
- The differences in life expectancy reflect the social and economic inequalities across the city.
- Health inequalities cannot be attributed to a single clinical or behavioural risk factor. They are influenced by social circumstances. Health will improve if people are supported to be physically active, eat and drink healthily and not smoke. However, these behaviours are significantly shaped by social circumstances such as income, housing, education, employment, spatial planning and transport all of which impact on people’s ability to exercise healthy choices.
- Loneliness and isolation and widening social inequalities are placing increased pressures on primary care services. There is evidence of increasing numbers of people seeking support for mental health issues much of which is associated with loneliness and isolation and distress due to money, employability, and housing worries.
- As people live longer, they live with chronic conditions. Multimorbidity will become the norm for the Edinburgh population. Mental health is a more common co-morbidity for people living in more deprived communities. Preventive actions can ensure people live healthily in their own homes rather than frequenting hospitals and other acute care services.
Biological, social and environmental determinants interact to influence people’s health and wellbeing (see Figure 1).[24] Measures of health must consider age, gender, geography, socio economic position, occupation, education and other determinants to capture the full range of health needs – and differences — across the population.
Figure 1: Dahlgren and Whitehead: the social determinants of health
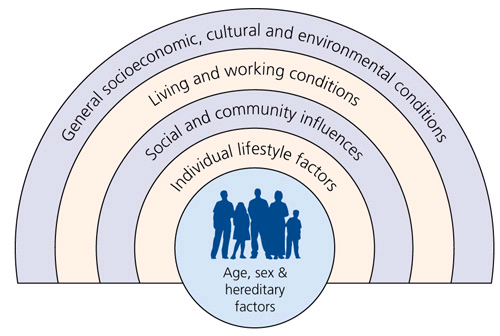
Inequalities develop over a life course as the result of ‘systematic, unfair differences in the health of the population that occur across social classes or population groups’. The ‘fundamental causes’ of health inequalities such as power and wealth affect the distribution of wider environmental influences such as the availability of jobs, good quality housing, education and learning opportunities, access to services, social status (see Figure 2).[25]
Figure 2: Fundamental causes of health inequalities
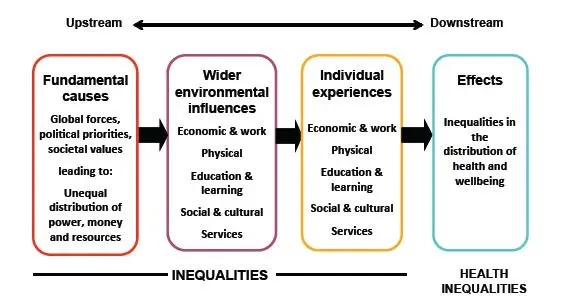
This results in differences in individual experiences of, for example, discrimination, prejudice, stigma, low income, and opportunities. These differences in individual experiences affect people’s health in three main ways:
- Differential exposure to environmental, cultural, socio-economic and educational influences that impact on health.
- The psychosocial consequences of differences in social status. There is now strong evidence that ‘status anxiety’ leads to psychological and physiological changes that affect health.
- The inequalities in health that are observed now will reflect not only current status but also differences in experiences at earlier stages in life. This is why interventions targeting families and the early years are so important.[26]
Inequalities in Edinburgh
Around 12% of Edinburgh’s population, or 60,000 people, live in areas categorised as among the most 20% deprived in Scotland. Within Edinburgh, there are more people living in the most deprived communities in the north east of the city. But only around a third of income deprived residents live in those areas of Edinburgh coded dark red in the mapping of Scottish Index of Multiple Deprivation (SIMD) in the city. In other words, around 65% (almost two thirds) of people who are income deprived live outside of the 20% most deprived areas of Edinburgh.[27].
Much of the analysis in this paper explores inequalities by SIMD quintile, due to the availability of data at this level. However, we can use our understanding of the inequalities between SIMD areas to also understand and respond to the issues that people living in poverty across the city are facing.
Figure 3: Scottish Index of Multiple Deprivation 2020 quintiles for Edinburgh
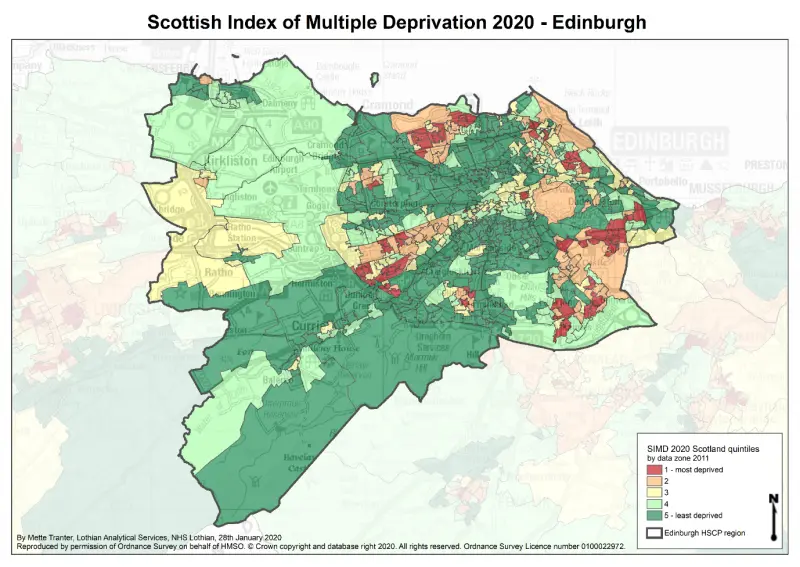
Inequalities in health arise because of inequalities in society; the circumstances into which people are born and grow have a significant impact on outcomes.[28] The accumulation of positive and negative effects on health and wellbeing contributes to widening inequalities across the life course. The influence of early years’ experience on later life health outcomes is well documented. In recent years the recognition that adverse childhood experience (ACEs) manifests as multiple negative health impacts has been a crucial extension of this knowledge.[29, 30]
Child health is indistinguishable from family or household health and it makes little sense to consider population health without reference to children and young people. Moreover, primary and community care services are part of the framework for getting it right for every child in the city so their needs have to be factored into this assessment.
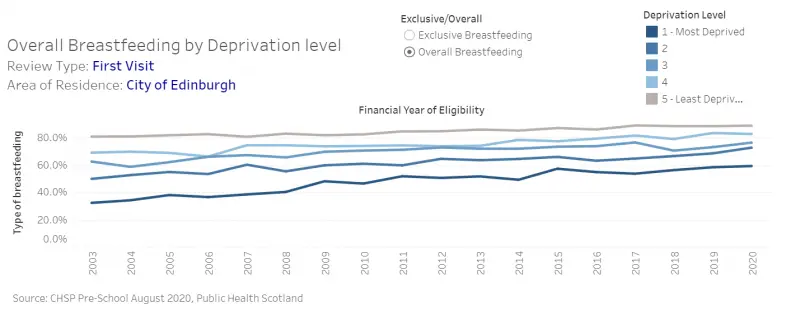
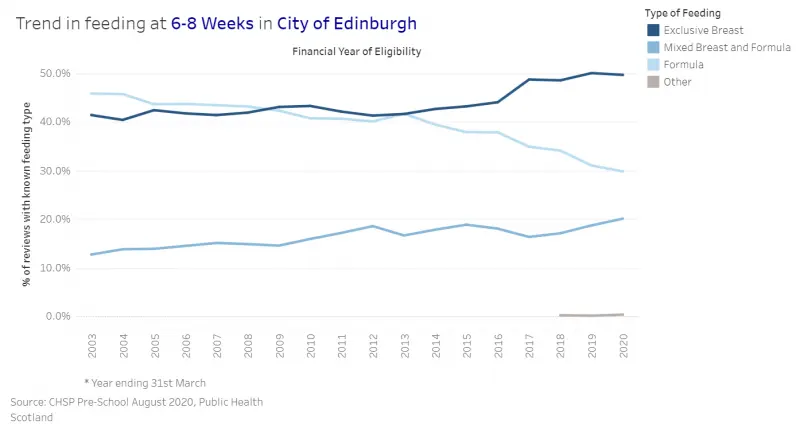
Inequalities in child health are evident early in the life course with babies from more deprived backgrounds being less likely to be breast fed and more likely to be exposed to second-hand smoke than those born to more affluent backgrounds.
Figure 4: Breastfeeding rates at six to eight week home visit in Edinburgh by SIMD quintile, 2003-2020
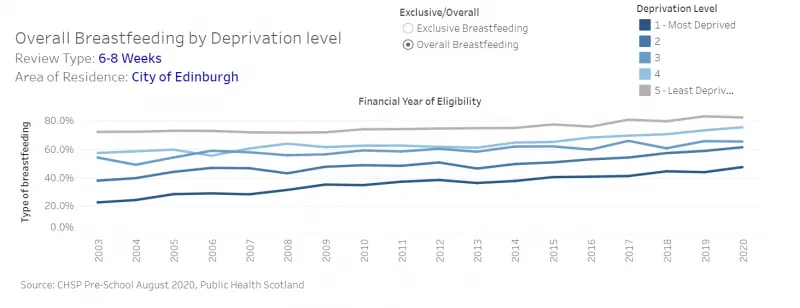
Weight at birth is a predictor of child and adult health outcomes. Those with lower birth weight are at increased risk of poorer cognitive skills and of developing cardiac disease in later life. In the year to 31 March 2019, 4.4% of babies born in Edinburgh were categorised as low birthweight. Although this is below the Scotland average, it amounts to 205 babies that year. The risk of low birth weight is higher among more deprived communities.
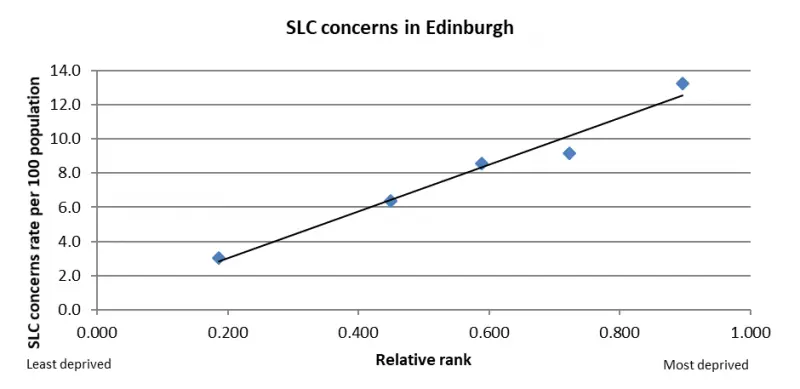
Speech and language acquisition is a key marker of early years development. Local research has demonstrated that socioeconomic factors account for development delays independent of delays associated with pre-term birth.[31] In Edinburgh there is a 13% difference in the rate of language acquisition between children living in the most and least deprived areas and children from more deprived communities are almost twice as likely to have a speech and language problem at 27-30 months.
The graph below shows the rate of speech and language concerns (SLC) per 100 population in relation to deprivation.
Figure 5: Slope Index of Inequality for speech and language concerns at 27-30 months for children in Edinburgh, 2014-18
Almost one in five children in Edinburgh were estimated to be living in poverty prior to the pandemic. Child poverty rates in Edinburgh have remained relatively unchanged in recent years, but are anticipated to rise sharply during 2021, while long-term trends suggest a continued steady increase throughout the next decade.
65% of all children in poverty live in a family where adults are in paid employment. People live in poverty in every area of this city – almost two thirds of people on very low incomes live in areas out with those parts of Edinburgh commonly described as ‘deprived’ or ‘disadvantaged’
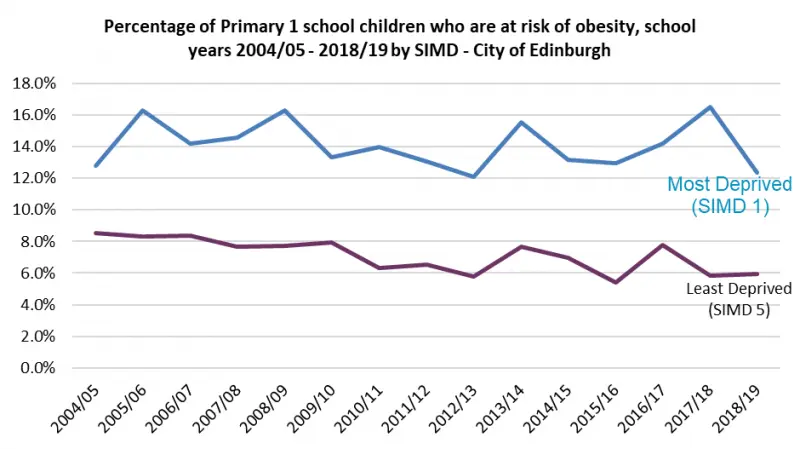
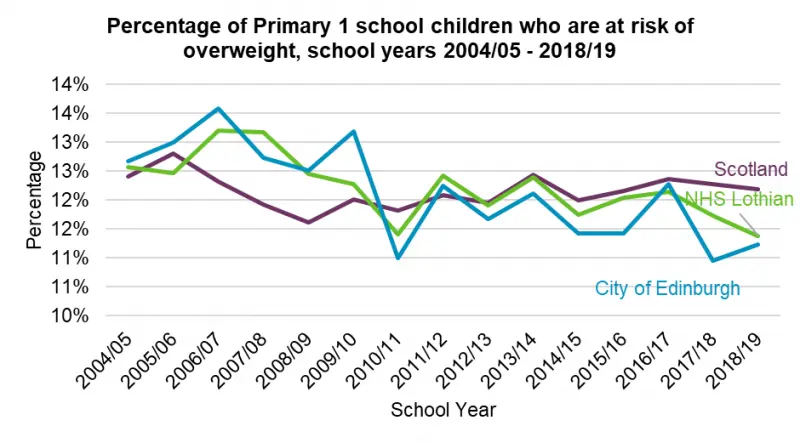
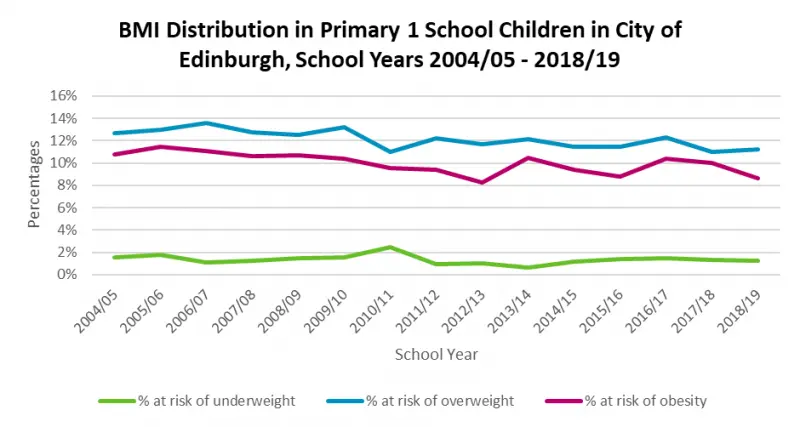
In the last ten years, the proportion of children in P1 who are overweight or at risk of obesity has remained broadly consistent at around 11%. However, children living in more deprived communities are consistently more likely to be categorised as at risk of overweight or obesity.
Figure 6: Percentage of Edinburgh P1 pupils at risk of obesity, 2004/5-2018/19
Child immunisation rates in Edinburgh are lower than the Scotland average.
| Local authority | Number in cohort | MMR1 | 4-in-1 | MMR2 | |||
|---|---|---|---|---|---|---|---|
| Number | Percentage | Number | Percentage | Number | Percentage | ||
| Edinburgh City | 4,749 | 4,523 | 95.2 | 4,344 | 91.5 | 4,341 | 91.4 |
| Scotland | 57,673 | 55,636 | 96.5 | 54,149 | 93.9 | 53,888 | 93.4 |
% completed primary and booster course by 6 years
- Born: 1 April 2014 to 31 March 2015
- Evaluation period: 1 April 2020 to 31 March 2021
- Source: SIRS
- Date: 10 May 2021
A similar pattern applies to uptake of vaccination for teenagers.
| Teenage Td/IPV booster | Teenage MenACWY | ||||||
|---|---|---|---|---|---|---|---|
| Number | Number offered vaccine in school year | Number immunised | Uptake rate (%) | Number immunised | Uptake rate (%) | ||
| Pupils in S3 | City of Edinburgh | 4,379 | 4,379 | 3,229 | 73.7 | 3,244 | 74.1 |
| Scotland | 56,450 | 49,966 | 39,789 | 79.6 | 39,873 | 79.8 | |
| Pupils in S6 | City of Edinburgh | 4,163 | n/a | 3,477 | 83.5 | 3,474 | 83.4 |
| Scotland | 55,939 | n/a | 48,472 | 86.7 | 48,580 | 86.8 |
Source: CHSP School/SIRS
Overall vaccination uptake rates in 2019-20 have been affected by the COVID-19 pandemic.
Teenage pregnancy rates[1] have decreased over the ten years to 2018 (the last year for which data are available). Edinburgh continues to have a consistently higher rate of teenage pregnancy than Scotland with higher rates being observed in the more deprived areas.
[1] Teenage pregnancy rates refers to pregnancies involving 13-15 year olds in this context
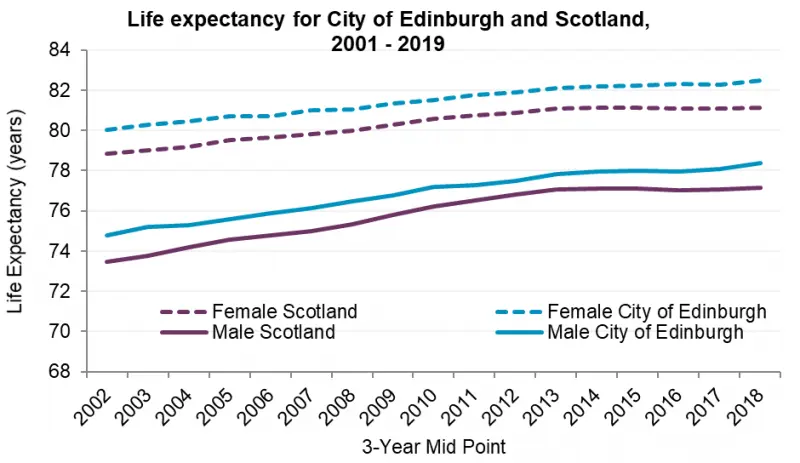
Life expectancy[2] in the city is consistently higher than the Scotland average. It increased steadily from 2002 until 2013. Since 2013 however, the improvements in life expectancy have slowed and in some parts of the city stalled altogether, which reflects the pattern that has emerged across Scotland.[32-34]
Figure 7 shows that male life expectancy in the city increased from 74.8 years to 78.4 years, and for females increased from 80 to 82.5. The rate of improvement for females in Edinburgh slowed compared to the improvement for males during the last five years which means the gap between male and female life expectancy has closed.
Figure 7: Edinburgh and Scotland life expectancy, 2002-2018 (Data represent the mid-point within the time period, i.e. the year 2011 represents the mid-point for 2010-2012)
Life expectancy, like most measures of health, is directly correlated to socioeconomic status. More affluent people tend to live longer lives and are more healthy during their lives. There is evidence of pronounced variation in mortality rates in Edinburgh with that trend manifest in the difference between life expectancy in most and least deprived communities: 14 years for males and 10 years for females (see Figure 8).[3]
Figure 8: Slope Index of Inequality for Edinburgh male and female life expectancy, 1999-2013
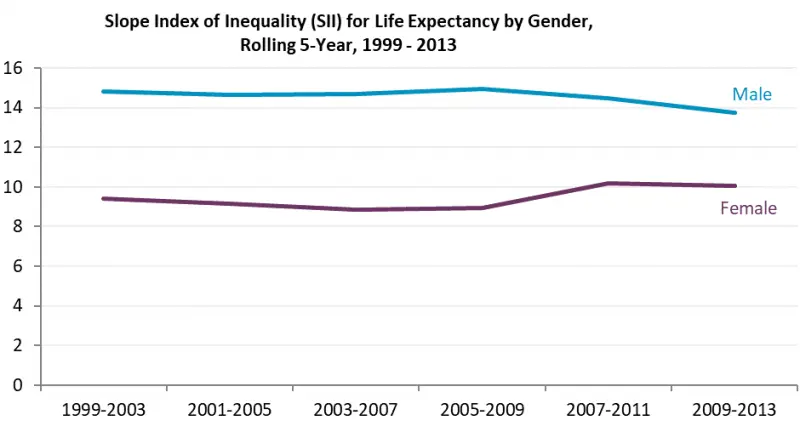
Within Edinburgh HSCP, there is a higher proportion of areas of multiple deprivation within the North East locality and life expectancy is lowest in this community. Table 3 also shows how improvements in life expectancy for both males and females has stalled in recent years.
| 2013 | 2014 | 2015 | 2016 | 2017 | 2018 | |
|---|---|---|---|---|---|---|
| Scotland | ||||||
| Males | 77.1 | 77.1 | 77.1 | 77.0 | 77.1 | 77.2 |
| Females | 81.1 | 81.1 | 81.1 | 81.1 | 81.1 | 81.1 |
| Edinburgh | ||||||
| Males | 77.9 | 78.0 | 78.0 | 78.0 | 78.1 | 78.4 |
| Females | 82.2 | 82.2 | 82.2 | 82.3 | 82.3 | 82.5 |
| North West | ||||||
| Males | 79.4 | 79.3 | 79.5 | 79.6 | 79.8 | – |
| Females | 83.0 | 83.2 | 83.5 | 83.6 | 83.6 | – |
| North East | ||||||
| Males | 75.3 | 75.5 | 75.6 | 75.9 | 76.1 | – |
| Females | 80.2 | 80.4 | 80.6 | 80.5 | 80.5 | – |
| South West | ||||||
| Males | 78.5 | 78.5 | 78.9 | 79.0 | 79.1 | – |
| Females | 82.9 | 82.9 | 83.1 | 83.2 | 83.3 | – |
| South East | ||||||
| Males | 78.3 | 78.6 | 78.5 | 78.3 | 78.3 | – |
| Females | 82.5 | 82.5 | 82.5 | 82.3 | 82.4 | – |
[2] Life expectancy at birth for an area is the number of years that a new-born baby would live if they experienced the age-specific mortality rates for that area, for the time period used, throughout their life. Life expectancy is a theoretical measure which reflects projections based on recent mortality rates throughout life, rather than a true prediction of the life expectancy of the local population. Life expectancy is calculated using National Records of Scotland mid-year population estimates and death registrations (by year of registration).
[3] The Slope Index of Inequality captures the difference in the average health status between a person in the highest socioeconomic group and a person in the lowest socioeconomic group.
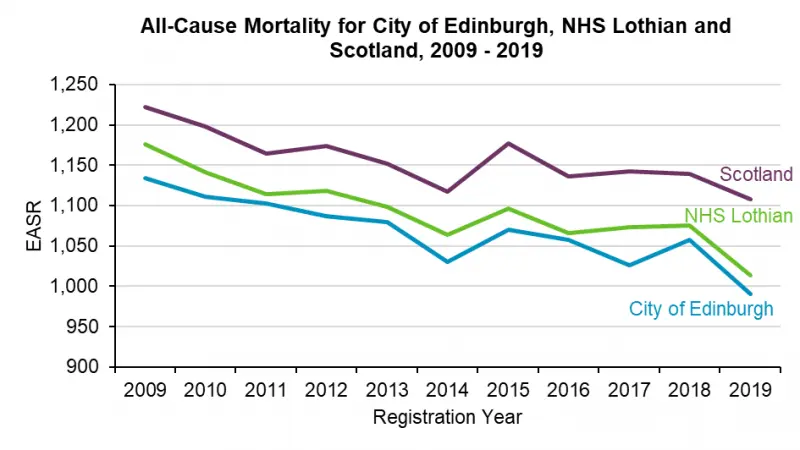
Mortality and morbidity[4], especially early mortality, increase with greater deprivation.[35] Figure 9 below shows Edinburgh had a consistently lower mortality rate from 2009 to 2019 compared to Scotland and NHS Lothian, and has continued to decrease over time to its lowest level in 2019.
Figure 9: All-cause mortality 2009-2019 for Edinburgh, Lothian and Scotland
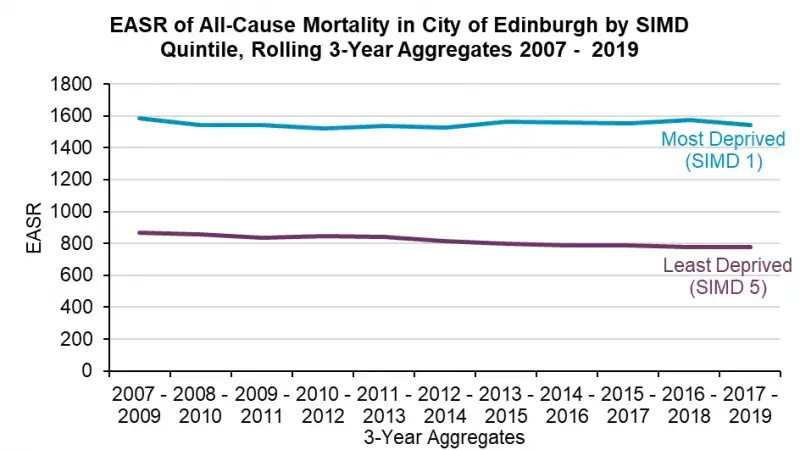
There is, however, significant inequality in mortality rates between people living in the most and least deprived areas in the city. Figure 10 shows that people living in the most deprived communities are dying at almost double the rate of people in the least deprived communities.
Figure 10: All-cause mortality for Edinburgh most and least deprived quintiles, 2007-2019
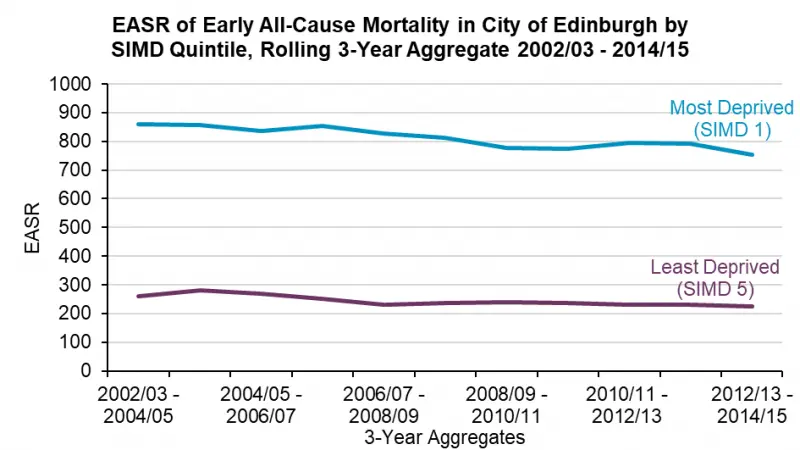
Early mortality rates are the number of deaths of people under 75 years observed over a specified time period; in effect, this subset of the overall death rate captures unfulfilled life expectancy. The Edinburgh premature mortality rate is consistently lower than the Scotland rate from 2009 to 2019. But the inequalities associated with premature mortality are even more pronounced than inequalities seen for all-cause mortality. There has been a greater decline in the premature mortality rate in the most deprived communities but the rate remains almost three times higher than seen in least deprived communities.
Figure 11: Early all-cause mortality for Edinburgh most and least deprived quintiles, 2002-2015
A significant component of early mortality are deaths associated with what has been termed the inclusion health population. Deaths of despair are most common among people aged 16-55 years and are associated with substance misuse, contact with the justice system, sex work and severe and enduring mental health problems.[36-38] Morbidity and mortality are notably worse among this population.[39-41]
Drug related deaths are a particular concern in Scotland. The most recent data relate to 2019. Drugs were the primary cause in 103 deaths in Edinburgh, which was an increase of 11% on the previous year and a 50% increase compared to 2014. These deaths are concentrated in the 30-50 age group and more common among males than females. There is a clear link to deprivation. Multiple drug use – mostly opioids — is an increasingly common cause of death but this population also experiences a wide range of chronic health conditions which will also contribute to early mortality. Deaths in these populations are driven by wider social determinants of health.
[4] Mortality rates are presented as European Age Standardised Rates (EASR) per 100,000 population. EASR takes account of differences in the age or sex structure of a population so that comparisons between areas can be meaningful. Otherwise, for example, an area might have a lower death rate simply because the proportion of younger people living there is higher than in another area.
While life expectancy is the average number of years those in a defined population are expected to live, healthy life expectancy (HLE) is the average number of years a person in a particular population is expected to live in a healthy state. People experiencing disabilities or limiting long term conditions tend to have poorer health overall.
Females in Edinburgh experience fewer years of good health than males. In recent years, there is evidence of a widening gap between males and females which appears to be a combination of improvements in male HLE and a worsening of female HLE. Although females have a higher life expectancy, they spend more than 20% of that life experiencing a low quality of life. For many people, increased life expectancy will be offset by years lived with disability.
| Males | Females | |||||
|---|---|---|---|---|---|---|
| Life expectancy (years) | Healthy life expectancy (years) | Percentage of life expectancy in good health | Life expectancy (years) | Healthy life expectancy (years) | Percentage of life expectancy in good health | |
| 2015-2017 | 78.0 | 65.0 | 83.4 | 82.3 | 65.1 | 79.1 |
| 2016-2018 | 78.1 | 65.4 | 83.8 | 82.3 | 63.9 | 77.6 |
| 2017-2019 | 78.4 | 66.3 | 84.6 | 82.5 | 65 | 78.8 |
The Scottish Burden of Disease study (2018) highlights how different diseases and conditions interact to affect people’s health and the impact this has on quality of life. Different disease combinations make a contribution to mortality and years of life lost compared with those diseases that contribute to years lived with a disability. A recent overview of health needs in the UK noted that ‘the application of effective preventive interventions, and advances in health care have led to a shift in the predominant share of the burden of ill-health worldwide from conditions causing premature mortality to conditions that cause disability.’[42] Years lived with a disability are of particular relevance when considering health and social care services.
The table below shows that cancer, cardiovascular disease, neurological disorders and respiratory diseases are the major contributors to mortality and years of life lost. Mental health disorders and musculoskeletal conditions have the greatest impact on years lived with a disability. In younger age groups, substance misuse contributes to disease burden while diseases of older age are dominated by mental health conditions and physically disabling conditions.[42] Preventative interventions across the life course are key to optimal health and social care.
| Mortality | Years of life lost | Years lived with a disability | Disability adjusted life years |
|---|---|---|---|
| Cancer | Cancer | Mental health disorders | Cancer |
| Cardiovascular diseases | Cardiovascular diseases | Musculoskeletal disorders | Cardiovascular diseases |
| Neurological disorders | Neurological disorders | Other non-communicable diseases | Neurological disorders |
| Chronic respiratory diseases | Chronic respiratory diseases | Neurological disorders | Mental health disorders |
| Diabetes, urogenital, blood & endocrine diseases | Substance use disorders | Cardiovascular diseases | Musculoskeletal disorders |
| Diarrhoea, lower respiratory & other common infectious diseases | Suicide, self-harm and interpersonal violence injuries | Diabetes, urogenital, blood & endocrine diseases | Other non-communicable diseases |
Source: Scottish Burden of Disease study, 2016[43]
The major disease categories in Edinburgh show a consistent trend where overall Edinburgh outcomes are better than Scotland and Lothian comparisons. Heart disease deaths have declined consistently for the last ten years. The same is true of various cancers.
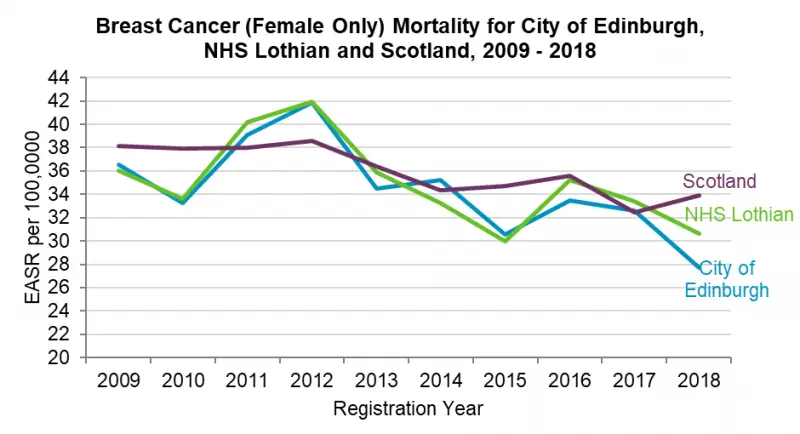
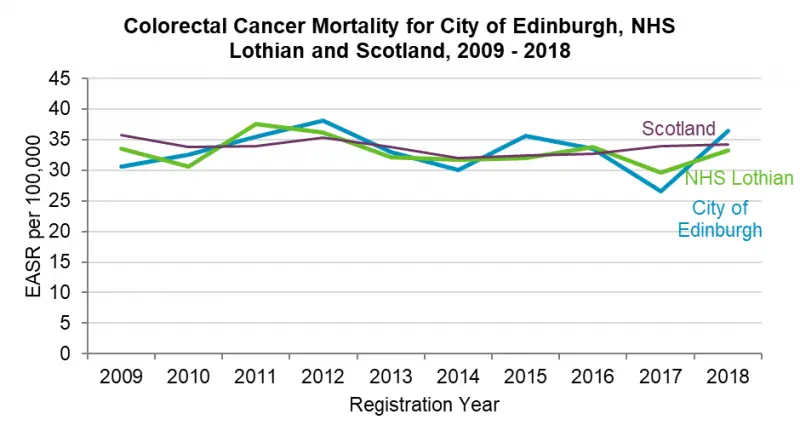
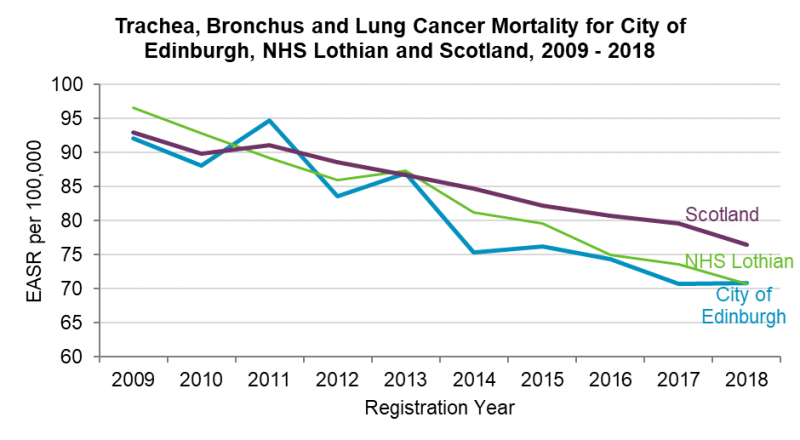
Over the last twenty years, the majority of cancers have shown improvement in survival rates five years post diagnosis. There has been a decrease in the European Age Standardised Rate (EASR) for Edinburgh residents for all age cancer mortality rates from 2008 to 2018. The mortality rate has been consistently below the Scottish average, although there was a slight increase in 2018.
The five most common cancers in Edinburgh in 2018 include cancers of the trachea, bronchus and lung; colorectal cancer; prostate cancer; pancreatic cancer; and breast cancer. Although the number of cancer diagnoses and deaths are projected to increase as the population ages, cancer incidence and mortality rates are projected to decline to 2035.[44-46] . It has been estimated that by 2040, 25% of all people aged 65 and older will be cancer survivors. Socioeconomic and environmental factors play a significant role in cancer burden. Research suggest that 41% of all cancers are attributable to modifiable risk factors.[47]
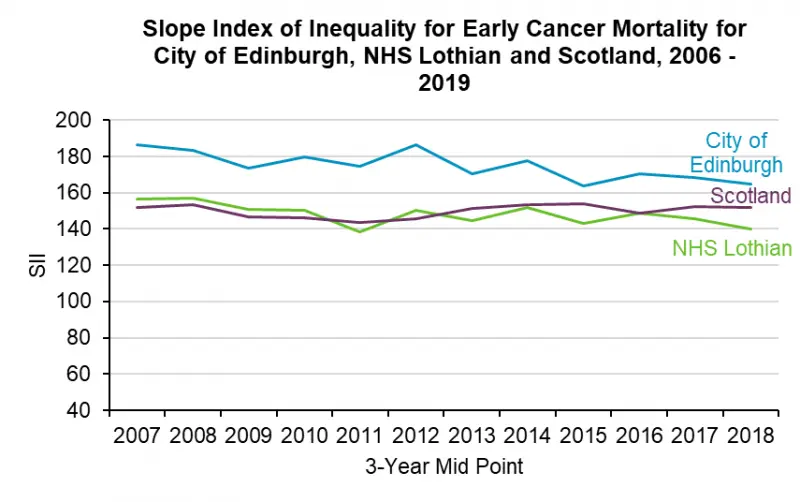
But there is a significant inequalities component that these average data disguise. The relative index of inequality shows that the gap between most and least deprived death rates for cancer (and heart disease) mortality are greater in Edinburgh than in Scotland or Lothian.
Figure 12: Slope Index of inequality for cancer mortality in Edinburgh, Lothian and Scotland, 2009-2019
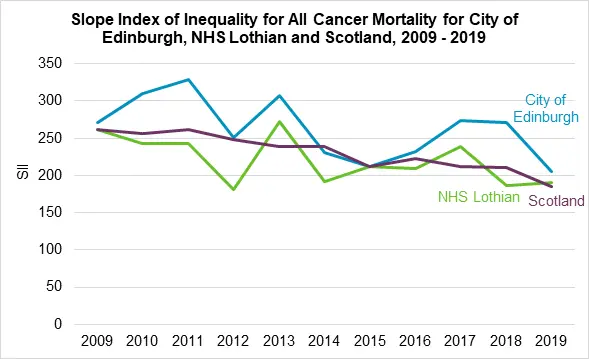
The socioeconomic gradient associated with heart disease and cancer means that higher income, occupational status and education are protective factors. Males continue to have higher rates of heart disease[48] but gender differences vary for cancers, with males more likely to develop bowel cancer but convergence of lung cancer incidence by gender.[49, 50]
Although clinical risk factors such as obesity, diabetes or hypertension and lifestyle factors such as smoking may increase coronary heart disease rates, inequalities will likely remain unless upstream factors associated with low socioeconomic status are addressed.
Screening programmes are vital early interventions. Increasing uptake among the whole population is key as long-term trends highlight clear disparities among population groups: males and people from more deprived communities are least likely to take up invitations for bowel screening (see Figures 13 and 14).
Figure 13: Bowel cancer screening uptake for males and females in Edinburgh, 2014-2018
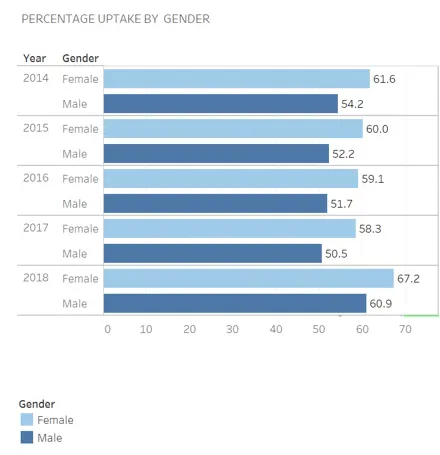
Figure 14: Bowel cancer screening uptake by SIMD quintile in Edinburgh, 2014-2018
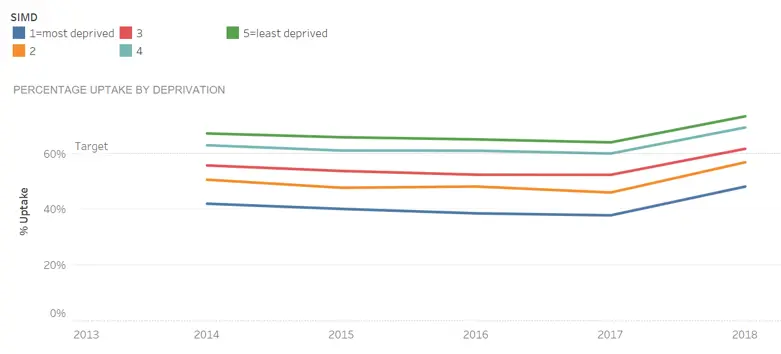
The proportion of positive tests from bowel screening is higher among people from more deprived communities and males. Uptake in most population groups is below the 60% target.
Cervical screening uptake is similar to bowel screening uptake insofar as there is a higher uptake in less deprived areas. Overall uptake of cervical screening is notably lower than the Scotland target of 80% in most population groups.
Figure 15: Cervical screening uptake in Edinburgh by SIMD quintile, 2018/19
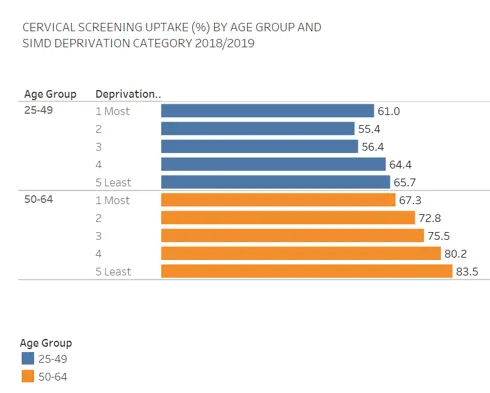
As the Scottish Burden of Disease study shows, mental health conditions are a significant component of morbidity. An extensive study of Scottish primary care records highlighted the prevalence of mental health problems and the extent to which socioeconomic deprivation is associated with earlier onset of physical and mental health problems. People from more deprived communities are also more likely to have a mental health diagnosis (see chart below).[51]
A recent study of British people born in 1970 suggests that one third had multimorbidity at ages 46-48 years. The most prevalent individual health outcomes were high-risk drinking (26.3%), recurrent back problems (20.9%), and mental health problems (19.1%) [28]
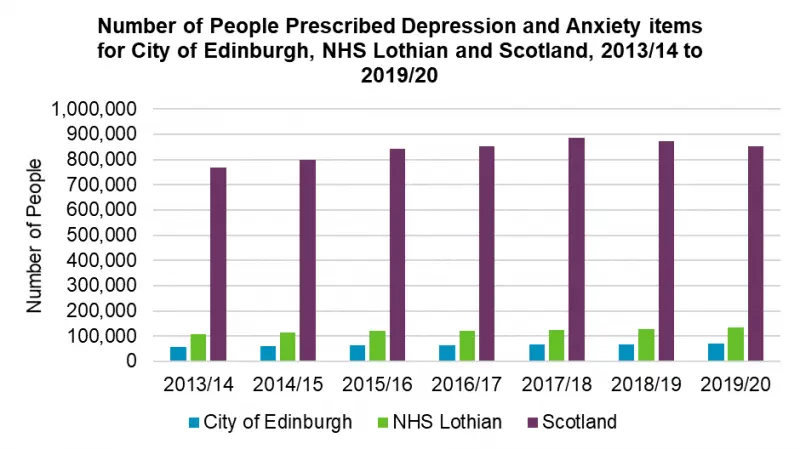
On an annual basis, almost 15% of Edinburgh’s population is prescribed drugs for treatment of anxiety and depression. This proportion is lower than Lothian and Scotland rates. But people living in most deprived areas are 10% more likely to be in receipt of one of these prescriptions.
Figure 16: Physical and mental health co-morbidities by SIMD
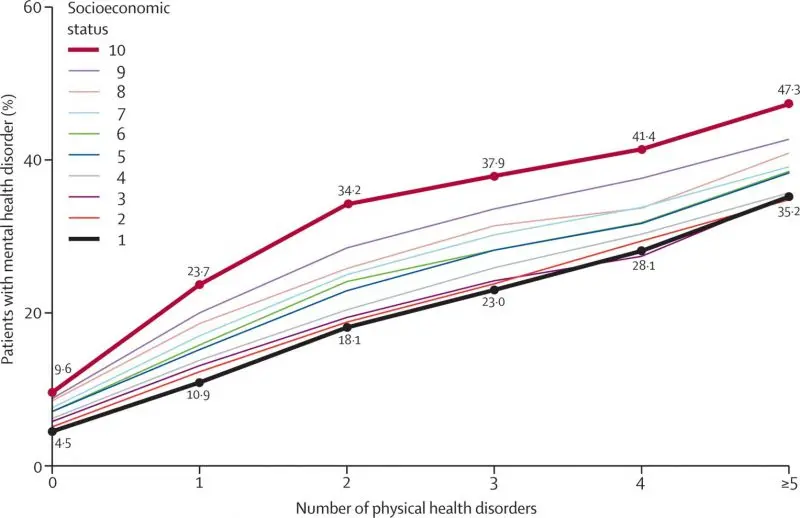
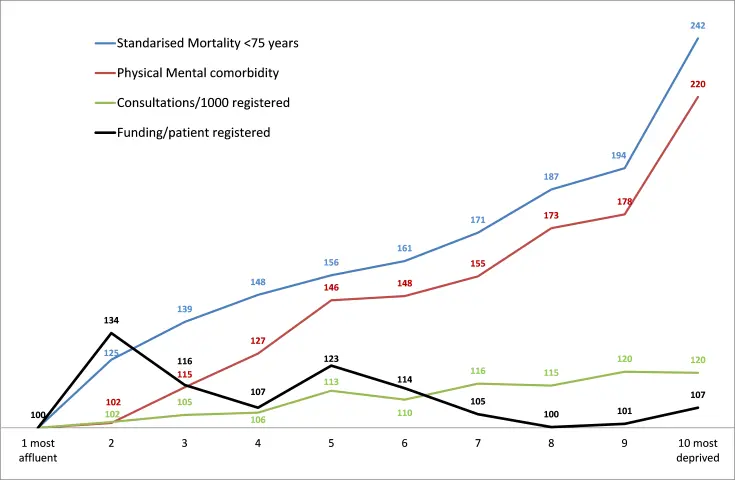
Primary care consultation rates are higher in areas with the greatest proportion of patients living in more deprived communities.[35, 52-54] A key role for organisations delivering health and social care is to mitigate and prevent health inequalities by providing healthcare and health improvement interventions in proportion to need. High quality, universal healthcare that is available to everyone with no or minimal cost is in itself important to mitigate and reduce health inequalities.
But within the universal service there are often other barriers that prevent some disadvantaged groups of people from receiving care. These include physical, social, environmental and practical barriers such as mismatch between service design and patient need, cultural differences between patients and staff, low expectations, poor experience, transport costs and lack of capacity where the need is highest. These all contribute to what is termed the ‘inverse care law’ – that quantity and quality of care may be poorest for those with the highest needs. There is evidence in Scotland that resources in our poorest communities are not sufficient for need.[35] There is some evidence to suggest that patients from more affluent backgrounds spend more time with doctors than patients from less affluent backgrounds.[52]
Figure 17: Mortality rates, morbidity rates, consultation rates and primary care funding in Scotland
The needs of an ageing population, particularly the management of dementia, multiple morbidity and frailty, also place a significant demand on primary and community care services.[55-57] As of 2018-29, prevalence of hypertension is 10% within the city, prevalence of depression was 6%, 5.5% for asthma and 4% for diabetes. These conditions significantly affect physical and mental wellbeing and quality of life as well as being associated with increased risk of hospitalisation. People living with long-term conditions are often prescribed many drugs. There is recognition of unintended health harms associated with polypharmacy.[58]
People who develop complex multiple morbidities also appear to be at greater risk of frailty in old age.[59, 60] There may be a link between early signs of frailty in middle age and frailty in later life. There is some evidence that strokes precipitate a quicker progression to multiple morbidities than diabetes and heart disease.[61]
People from these communities are most likely to have unscheduled hospital admissions.[4] Many of these hospital admissions are potentially preventable. Potentially preventable admissions are defined as conditions that can be managed with timely and effective treatment in the outpatient setting. There are 19 conditions defined as ‘potentially preventable’, such as COPD, angina and diabetes complications. There are more than 7,000 potentially preventable hospital admissions in Edinburgh annually.
Immunisation and vaccination programmes are vital early interventions. Ensuring uptake of childhood immunisations, flu vaccinations and the shingles booster for older people are key.
It is important to understand the distinction between loneliness and isolation. Age UK defines ‘isolation’ as separation from social or familial contact, community involvement, or access to services, while ‘loneliness’ can be understood as an individual’s personal, subjective sense of lacking these things. It is therefore possible to be isolated without being lonely, and to be lonely without being isolated.
Loneliness and isolation impact physical, mental, and social wellbeing across the life course and can be as harmful to health as smoking 15 cigarettes per day. Loneliness and isolation are associated with higher all-cause mortality for both sexes.[62-65]. There is a clear link between loneliness and isolation and care utilisation. 20% of consultations with primary care are thought to be for social rather than medical reasons. There is an increased demand on primary care services for support with mental wellbeing much of which is associated with depression due to social isolation.
Consultation for the Edinburgh Locality Plans in 2018 highlighted isolation and loneliness as major issues for the local population.
Race, migration status, disability and gender are other factors associated with poor health. Although overall mortality for people from some black and ethnic minority populations is similar or better than the white Scottish population, there are aspects of health – notably cardiovascular and diabetes – where access to services and outcomes are worse, particularly for people from south Asian populations.[66-69]
A study of the Health and Care Needs of People from Minority Ethnic Communities in Edinburgh conducted in 2018 reiterated the disease specific issues facing people from black and ethnic minority communities but also flagged a range of social issues that must be considered to understand the complexity and variety of population health needs. So, for example, Pakistani men in Scotland have higher rates of heart attacks, respiratory disease and hospital admissions for asthma compared to other ethnic groups; south Asian females have a lower rate of uptake for breast cancer screening; and suicide rates among the Polish community in Scotland are higher than the Scottish average.
Social factors that contribute to health care needs for people from black and ethnic minority populations include racism and hate crime, social isolation and low income and unemployment. The report emphasises the need for staff training including cultural sensitivity, recognition of the role of the Third Sector in supporting people from ethnic minority communities, effective community engagement and the importance of effective approaches to prevention including overcoming isolation.[70]
Harm from tobacco
Smoking is one of the leading causes of preventative illness and premature death. Smoking is not a lifestyle choice but rather a relapsing long-term condition, often the result of wider social drivers and is closely linked to social deprivation. Half of all smokers die prematurely losing on average ten years of life. Harm from tobacco is concentrated in more disadvantaged communities and groups including those living in more deprived areas and those with mental illness.
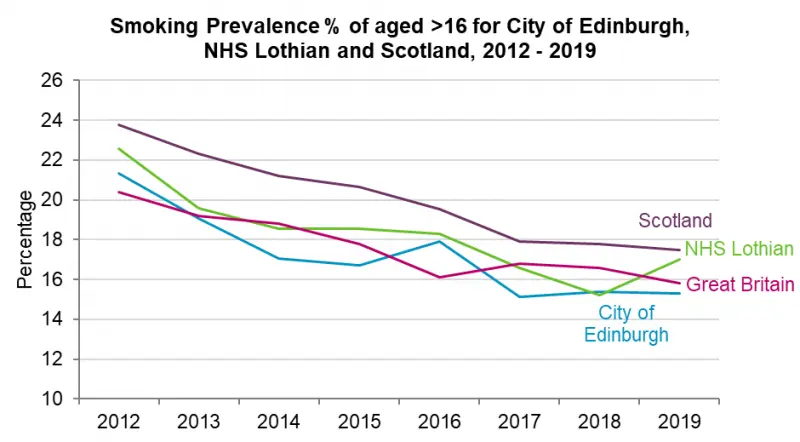
Edinburgh’s smoking rates show a continued decline over time and rates are better than comparator areas. But there is a pronounced association with socioeconomic position which means that smoking is a contributory factor to health inequalities.
| 2012/13 | 2013/14 | 2014/15 | 2015/16 | 2016/17 | 2017/18 | |
|---|---|---|---|---|---|---|
| City of Edinburgh | 330.9 | 316.8 | 291.9 | 290.8 | 286.1 | 271.9 |
| NHS Lothian | 342.1 | 328.9 | 311.1 | 301.8 | 298.8 | 283.7 |
| Scotland | 370.7 | 359.3 | 351.9 | 344.6 | 336.9 | 327.8 |
Age-sex standardised rate per 100,000, calendar years; 2-year aggregates
Tobacco related illnesses are leading causes of preventable death and healthcare use. Smokers see their GP over a third more often than non-smokers and they are more likely to experience hospital admissions.
Smoking is the single most modifiable risk factor in pregnancy and is associated with a range of poorer health outcomes for the women and their unborn babies. Smoking in pregnancy is one of the key risk factors for low birthweight.
The proportion of women smoking during pregnancy is lower in Edinburgh than NHS Lothian and Scotland average. Nevertheless, in 2019/20 8.3% (376) women in Edinburgh smoked during pregnancy. National data also show that women in the most deprived communities in Edinburgh are 139% more likely to smoke during pregnancy than average.
The table shows the proportion of women smoking during pregnancy in Edinburgh with comparisons for NHS Lothian and Scotland.
| 2012/13 | 2013/14 | 2014/15 | 2015/16 | 2016/17 | 2017/18 | 2018/19 | 2019/20 | ||
|---|---|---|---|---|---|---|---|---|---|
| City of Edinburgh | n | 729 | 667 | 623 | 583 | 561 | 506 | 441 | 376 |
| % | 13.1 | 12.3 | 11.7 | 11.3 | 11.1 | 10.4 | 9.4 | 8.3 | |
| NHS Lothian | n | 1,549 | 1,451 | 1,378 | 1,295 | 1,225 | 1,123 | 1,017 | 895 |
| % | 16.8% | 15.8 | 15.0 | 14.2 | 13.7 | 12.9 | 12.1 | 11 | |
| Scotland | n | 10,340 | 9,807 | 9,164 | 8,559 | 7,864 | 7,399 | 6,971 | 6,444 |
| % | 19.4 | 18.5 | 17.4 | 16.3 | 15.4 | 14.9 | 14.6 | 13.9 |
Overweight, obesity and physical inactivity
Although Edinburgh’s population rate of obesity is lower than Edinburgh and Scotland rates, almost one in five adults in the city have a Body Mass Index above 30. Obesity and overweight are socially patterned and these risk factors again weigh most heavily in the most deprived communities.
Physical activity rates show a similar trend. But it is important to note that social circumstances are key influences on activity rates and healthy weight: better income, jobs and education are associated with more activity and healthy weight.
Harm from Alcohol
Alcohol is more affordable and available than at any time in recent history, and while many people who drink would consider that they do so without causing harm to themselves or others, there is a strong and growing evidence base for the harmful impact alcohol misuse can have on individuals, families and communities.
Levels of alcohol-related harm in relation to crime, community safety, child welfare, health and wellbeing are concerning, and have a greater affect in our most deprived communities, contributing to inequalities across Edinburgh.
Alcohol specific death rates in Edinburgh show a long-term decline; however, they are higher than the Lothian average and have shown a slight uptick in the past ten years. National legislation for minimum unit pricing has contributed to a decline overall in alcohol deaths. But a suite of interventions is still necessary to reduce negative health outcomes associated with alcohol.
Alcohol specific death rates in Scotland are considerably higher than other UK nations. The Edinburgh rate is higher than rates for England, Wales and Northern Ireland. Between 2012 and 2019, rates of alcohol-specific deaths in the UK remained stable, with no statistically significant differences in the year-on-year rates. However, the rates seen in 2020 and 2021 are statistically significantly higher than 2019 and any other year since the start of the Office for National Statistics time series in 2001. This rise is likely to be the result of increased alcohol consumption since the onset of the COVID-19 pandemic, with alcoholic liver disease the leading cause of these deaths. Research has suggested that people who were already drinking at higher levels before the pandemic were most likely to have increased their alcohol consumption during this period. 71
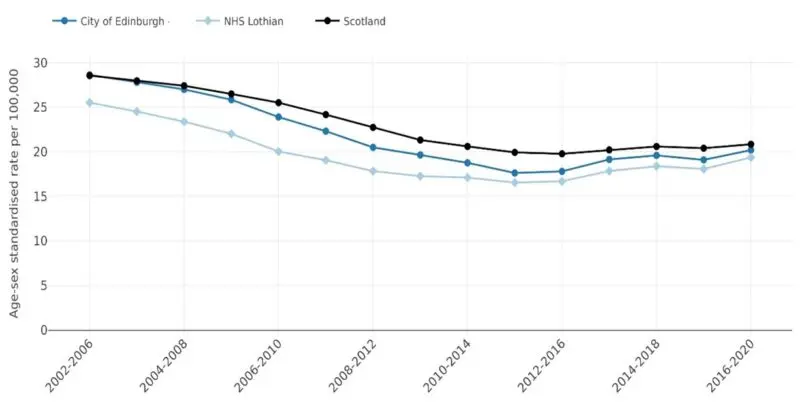
Figure 18 shows alcohol-specific deaths in each of Edinburgh, Lothian and Scotland in five year aggregates from 2002 to 2020. Over the period the rate has fallen overall for all three, although the second half shows a plateauing and a slight increase, particularly in NHS Lothian. Unlike in the UK data, the effects of the pandemic on alcohol-related harm are not yet evident in the Scottish data, though we may see this appear as more recent data is released.
Figure 18: Alcohol-specific deaths in Edinburgh, Lothian and Scotland 2002-2020
Excessive use of alcohol is linked to a range of physical and mental health problems, as well as accidental injury and premature mortality. Medical conditions linked with alcohol use include high blood pressure, liver disease, stroke, cancer and brain damage.
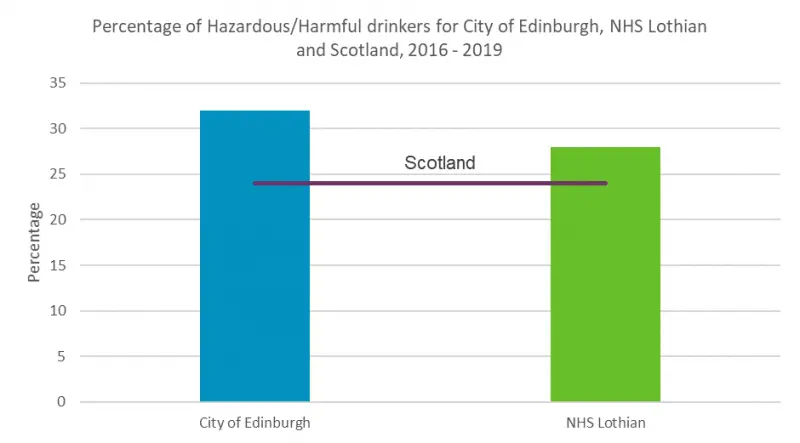
In recent years, the proportion of Edinburgh residents drinking at hazardous rates has been higher than Lothian and Scotland, as shown in figure 19. The graph below shows that the percentage of hazardous drinkers in Edinburgh (32%) is higher than the Scotland (28%) average.
Figure 19: Percentage adults harmful drinking in Edinburgh, Lothian and Scotland, 2016-2019
This data appendix provides more detail about specific diseases and risk factors discussed above.
- Marmot, M. and J. Allen, COVID-19: exposing and amplifying inequalities. Journal of Epidemiology and Community Health, 2020. 74(9): p. 681-682.
- Marmot, M., et al., Build Back Fairer: The COVID-19 Marmot Review. The Pandemic, Socioeconomic and Health Inequalities in England. 2020, Institute of Health Equity: London.
- Wyper, G.M.A., et al., Inequalities in Population Health Loss by Multiple Deprivation: COVID-19 and Pre-pandemic All-cause Disability-adjusted Life Years (dalys) in Scotland. SocArXiv, 2021.
- Burström, B. and W. Tao, Social determinants of health and inequalities in COVID-19. European Journal of Public Health, 2020.
- Mutambudzi, M., et al., Occupation and risk of severe COVID-19: prospective cohort study of 120,075 UK Biobank participants. medRxiv, 2020: p. 2020.05.22.20109892.
- Williamson, E., et al., OpenSAFELY: factors associated with COVID-19-related hospital death in the linked electronic health records of 17 million adult NHS patients. medRxiv, 2020: p. 2020.05.06.20092999.
- Williamson, E.J., et al., Factors associated with COVID-19-related death using OpenSAFELY. Nature, 2020. 584(7821): p. 430-436.
- Harrison, E., et al., Ethnicity and Outcomes from COVID-19: The ISARIC CCP-UK Prospective Observational Cohort Study of Hospitalised Patients. SSRN Electronic Journal, 2020.
- Aldridge, R., et al., Black, Asian and Minority Ethnic groups in England are at increased risk of death from COVID-19: indirect standardisation of NHS mortality data [version 1; peer review: awaiting peer review]. Wellcome Open Research, 2020. 5(88).
- Ayoubkhani, D., et al., Epidemiology of post-COVID syndrome following hospitalisation with coronavirus: a retrospective cohort study. medRxiv, 2021: p. 2021.01.15.21249885.
- Gruer, L.D., et al., Complex differences in infection rates between ethnic groups in Scotland: a retrospective, national census-linked cohort study of 1.65 million cases. Journal of Public Health, 2021.
- Mathur, R., et al., Ethnic differences in SARS-CoV-2 infection and COVID-19-related hospitalisation, intensive care unit admission, and death in 17 million adults in England: an observational cohort study using the OpenSAFELY platform. The Lancet, 2021. 397(10286): p. 1711-1724.
- National Records of Scotland, Deaths involving coronavirus (COVID-19) in Scotland, Week 27 (05-11 July). 2021, NRS: Edinburgh.
- Ayoubkhani, D., et al., Post-covid syndrome in individuals admitted to hospital with covid-19: retrospective cohort study. BMJ, 2021. 372: p. n693.
- Sigfrid, L., et al., Long Covid in adults discharged from UK hospitals after Covid-19: A prospective, multicentre cohort study using the ISARIC WHO Clinical Characterisation Protocol. medRxiv, 2021: p. 2021.03.18.21253888.
- Drake, T.M., et al., Characterisation of in-hospital complications associated with COVID-19 using the ISARIC WHO Clinical Characterisation Protocol UK: a prospective, multicentre cohort study. The Lancet, 2021. 398(10296): p. 223-237.
- Jia, R., et al., Mental health in the UK during the COVID-19 pandemic: cross-sectional analyses from a community cohort study. BMJ Open, 2020. 10(9): p. e040620.
- Banks, J. and X. Xu, The mental health effects of the first two months of lockdown and social distancing during the Covid-19 pandemic in the UK, in Working Papers. 2020, Institute for Fiscal Studies: London.
- Niedzwiedz, C.L., et al., Mental health and health behaviours before and during the initial phase of the COVID-19 lockdown: longitudinal analyses of the UK Household Longitudinal Study. Journal of Epidemiology and Community Health, 2020: p. jech-2020-215060.
- Pierce, M., et al., Mental Health Before and During the COVID-19 Pandemic: A Longitudinal Probability Sample Survey of the UK Population.
- Raisi-Estabragh, Z., et al., Greater risk of severe COVID-19 in Black, Asian and Minority Ethnic populations is not explained by cardiometabolic, socioeconomic or behavioural factors, or by 25(OH)-vitamin D status: study of 1326 cases from the UK Biobank. Journal of Public Health, 2020.
- Sze, S., et al., Ethnicity and clinical outcomes in COVID-19: A systematic review and meta-analysis. EClinicalMedicine.
- Razai, M.S., et al., Mitigating ethnic disparities in covid-19 and beyond. BMJ, 2021. 372: p. m4921.
- Dahlgren, G. and M. Whitehead, Policies and strategies to promote social equity in health. 1991, Institute for Future Studies: Stockholm.
- Macintyre, S., Inequalities in health in Scotland: what are they and what can we do about them?, in MRC Social and Public Health Sciences Unit Occasional Papers. 2007, MRC Social and Public Health Sciences Unit: Glasgow.
- Braveman, P. and L. Gottlieb, The social determinants of health: it’s time to consider the causes of the causes. Public health reports (Washington, D.C. : 1974), 2014. 129 Suppl 2(Suppl 2): p. 19-31.
- Robertson, L., Poverty in Edinburgh: The Key Issues. 2019, Edinburgh Poverty Commission: Edinburgh.
- Gondek, D., et al., Prevalence and early-life determinants of mid-life multimorbidity: evidence from the 1970 British birth cohort. BMC Public Health, 2021. 21(1): p. 1319.
- Bellis, M.A., et al., Measuring mortality and the burden of adult disease associated with adverse childhood experiences in England: a national survey. Journal of Public Health, 2014.
- Hughes, K., et al., The effect of multiple adverse childhood experiences on health: a systematic review and meta-analysis. The Lancet Public Health, 2017. 2(8): p. e356-e366.
- Ene, D., et al., Associations of Socioeconomic Deprivation and Preterm Birth With Speech, Language, and Communication Concerns Among Children Aged 27 to 30 Months. JAMA Network Open, 2019. 2(9): p. e1911027-e1911027.
- Ramsay, J., et al., How have changes in death by cause and age group contributed to the recent stalling of life expectancy gains in Scotland? Comparative decomposition analysis of mortality data, 2000–2002 to 2015–2017. BMJ Open, 2020. 10(10): p. e036529.
- Fenton, L., et al., Socioeconomic inequality in recent adverse all-cause mortality trends in Scotland. Journal of Epidemiology and Community Health, 2019. 73(10): p. 971-974.
- Fenton, L., et al., Recent adverse mortality trends in Scotland: comparison with other high-income countries. bioRxiv, 2019: p. 542449.
- McLean, G., et al., General practice funding underpins the persistence of the inverse care law: cross-sectional study in Scotland. British Journal of General Practice, 2015. 65(641): p. e799-e805.
- Walsh, D., et al., Deaths from ‘diseases of despair’ in Britain: comparing suicide, alcohol-related and drug-related mortality for birth cohorts in Scotland, England and Wales, and selected cities. Journal of Epidemiology and Community Health, 2021: p. jech-2020-216220.
- Allik, M., et al., Deaths of despair: cause-specific mortality and socioeconomic inequalities in cause-specific mortality among young men in Scotland. International Journal for Equity in Health, 2020. 19(1): p. 215.
- Koltai, J., et al., Deaths of Despair and Brexit Votes: Cross-Local Authority Statistical Analysis in England and Wales. American Journal of Public Health. 0(0): p. e1-e6.
- Tweed, E.J., et al., Health of people experiencing co-occurring homelessness, imprisonment, substance use, sex work and/or severe mental illness in high-income countries: a systematic review and meta-analysis. Journal of Epidemiology and Community Health, 2021: p. jech-2020-215975.
- Aldridge, R.W., et al., Morbidity and mortality in homeless individuals, prisoners, sex workers, and individuals with substance use disorders in high-income countries: a systematic review and meta-analysis. The Lancet.
- Luchenski, S., et al., What works in inclusion health: overview of effective interventions for marginalised and excluded populations. The Lancet.
- McKee, M., et al., The changing health needs of the UK population. The Lancet, 2021. 397(10288): p. 1979-1991.
- Scottish Public Health Observatory. Scottish Burden of Disease Study 2016: local area burden of disease profiles for disease groups. [Spreadsheet] 2021 18 March 2021 [cited 2021 05 August]; An excel workbook detailing burden of disease estimates (DALYs, YLD, YLL and deaths) for 21 broad disease groupings, stratified by: Local authority, Gender, Age-group]. Available from: https://www.scotpho.org.uk/comparative-health/burden-of-disease/sbod-local-2016/.
- Quaresma, M., M.P. Coleman, and B. Rachet, 40-year trends in an index of survival for all cancers combined and survival adjusted for age and sex for each cancer in England and Wales, 1971–2011: a population-based study. The Lancet, 2015. 385(9974): p. 1206-1218.
- Maddams, J., M. Utley, and H. Moller, Projections of cancer prevalence in the United Kingdom, 2010-2040. Br J Cancer, 2012. 107(7): p. 1195-1202.
- Smittenaar, C.R., et al., Cancer incidence and mortality projections in the UK until 2035. British Journal of Cancer, 2016. 115(9): p. 1147-1155.
- Brown, K.F., et al., The fraction of cancer attributable to modifiable risk factors in England, Wales, Scotland, Northern Ireland, and the United Kingdom in 2015. British Journal of Cancer, 2018. 118(8): p. 1130-1141.
- Scottish Public Health Observatory. Heart disease: Scottish data. 2021 [cited 2021 04 August]; Available from: https://www.scotpho.org.uk/health-wellbeing-and-disease/coronary-heart-disease/data/scottish-data/.
- Scottish Public Health Observatory. Colorectal cancer: key points. 2021 [cited 2021 04 August]; Available from: https://www.scotpho.org.uk/health-wellbeing-and-disease/cancer-colorectal/key-points/.
- Scottish Public Health Observatory. Lung cancer: key points. 2021 [cited 2021 04 August ]; Available from: https://www.scotpho.org.uk/health-wellbeing-and-disease/cancer-lung/key-points/.
- Barnett, K., et al., Epidemiology of multimorbidity and implications for health care, research, and medical education: a cross-sectional study. Lancet, 2012. 380(9836): p. 37-43.
- Mercer, S.W., et al., Multimorbidity and Socioeconomic Deprivation in Primary Care Consultations. The Annals of Family Medicine, 2018. 16(2): p. 127-131.
- Mercer, S.W., et al., Multimorbidity and the inverse care law in primary care. BMJ, 2012. 344: p. e4152.
- Mercer, S.W. and G.C.M. Watt, The inverse care law: clinical primary care encounters in deprived and affluent areas of Scotland. Annals of Family Medicine, 2007. 5(6): p. 503-10.
- Buckinx, F., et al., Burden of frailty in the elderly population: perspectives for a public health challenge. Archives of Public Health, 2015. 73(1): p. 19.
- Kingston, A., et al., Projections of multi-morbidity in the older population in England to 2035: estimates from the Population Ageing and Care Simulation (PACSim) model. Age and Ageing, 2018.
- Kingston, A., A. Comas-Herrera, and C. Jagger, Forecasting the care needs of the older population in England over the next 20 years: estimates from the Population Ageing and Care Simulation (PACSim) modelling study. The Lancet Public Health, 2018. 3(9): p. e447-e455.
- Zaninotto, P., et al., Polypharmacy is a risk factor for hospital admission due to a fall: evidence from the English Longitudinal Study of Ageing. BMC Public Health, 2020. 20(1): p. 1804.
- Hanlon, P., et al., Frailty and pre-frailty in middle-aged and older adults and its association with multimorbidity and mortality: a prospective analysis of 493 737 UK Biobank participants. The Lancet Public Health, 2018. 3(7): p. e323-e332.
- Brunner, E.J., et al., Midlife contributors to socioeconomic differences in frailty during later life: a prospective cohort study. The Lancet Public Health, 2018. 3(7): p. e313-e322.
- Xu, X., et al., Progression of diabetes, heart disease, and stroke multimorbidity in middle-aged women: A 20-year cohort study. PLOS Medicine, 2018. 15(3): p. e1002516.
- Steptoe, A., A. Deaton, and A.A. Stone, Subjective wellbeing, health, and ageing. The Lancet, 2014(0).
- Steptoe, A., et al., Social isolation, loneliness, and all-cause mortality in older men and women. Proceedings of the National Academy of Sciences, 2013. 110(15): p. 5797-5801.
- Cacioppo, J.T. and S. Cacioppo, Social Relationships and Health: The Toxic Effects of Perceived Social Isolation. Social and Personality Psychology Compass, 2014. 8(2): p. 58-72.
- Conklin, A.I., et al., Social relationships and healthful dietary behaviour: Evidence from over-50s in the EPIC cohort, UK. Social Science & Medicine, 2014. 100(0): p. 167-175.
- Bhopal, R., et al., Risk of respiratory hospitalization and death, readmission and subsequent mortality: Scottish health and ethnicity linkage study. European Journal of Public Health, 2015.
- Bhopal, R.S., et al., Mortality, ethnicity, and country of birth on a national scale, 2001–2013: A retrospective cohort (Scottish Health and Ethnicity Linkage Study). PLOS Medicine, 2018. 15(3): p. e1002515.
- Fischbacher, C.M., et al., Measures of socioeconomic position are not consistently associated with ethnic differences in cardiovascular disease in Scotland: methods from the Scottish Health and Ethnicity Linkage Study (SHELS). International Journal of Epidemiology, 2014. 43(1): p. 129-139.
- Gruer, L., et al., Life expectancy of different ethnic groups using death records linked to population census data for 4.62 million people in Scotland. Journal of Epidemiology and Community Health, 2016.
- Cunningham, E., et al., Edinburgh Health and Social Care Partnership Joint Strategic Needs Assessment Health and Care Needs of People from Minority Ethnic Communities Final Report April 2018. 2018, Edinburgh IJB: Edinburgh.
- Office for National Statistics. Alcohol-specific deaths in the UK: registered in 2021. Available from https://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/deaths/bulletins/alcoholspecificdeathsintheuk/2021registrations

